Gestational diabetes, a temporary condition during pregnancy, impacts blood sugar levels and requires careful management for maternal and fetal health.
What is gestational diabetes, and how is it diagnosed?
Gestational diabetes, a condition that develops during pregnancy, can pose risks to both the mother and the baby. This article explores the causes, risks, and effective management of gestational diabetes, providing essential information for expectant mothers.
What Is Gestational Diabetes?
Gestational diabetes is a temporary form of diabetes that occurs during pregnancy. It affects how the body processes sugar (glucose), leading to elevated blood sugar levels. This condition typically develops in the second half of pregnancy and can affect the health of both the mother and the baby.
Causes and Risk Factors
The exact cause of gestational diabetes is not fully understood, but several factors increase the risk of developing it. These risk factors include:
- Obesity: Women with a higher body mass index (BMI) are more likely to develop gestational diabetes.
- Family History: A family history of diabetes can increase the risk.
- Age: Women over the age of 25 are at a higher risk.
- Previous Gestational Diabetes: If a woman had gestational diabetes in a previous pregnancy, the risk is higher in subsequent pregnancies.
Impact on Mother and Baby
Gestational diabetes can have various effects on both the mother and the baby. For the mother, it can lead to:
- Increased risk of preeclampsia (high blood pressure during pregnancy).
- A higher chance of requiring a cesarean section (C-section) during delivery.
For the baby, the risks include:
- Macrosomia (large birth weight), which can lead to birth complications.
- Hypoglycemia (low blood sugar) after birth.
- An increased risk of developing type 2 diabetes later in life.
Diagnosis and Monitoring
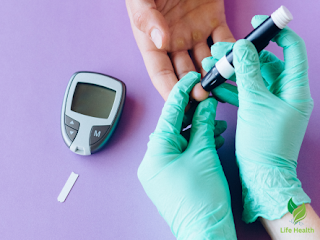
Prenatal care typically includes screening for gestational diabetes, usually between weeks 24 and 28 of pregnancy. This involves a glucose challenge test, followed by a glucose tolerance test if the initial test indicates high blood sugar levels.
Monitoring glucose levels is a crucial part of managing gestational diabetes. Many women can control their blood sugar through dietary changes and regular exercise. For some, medication or insulin may be necessary.
Management and Treatment
The management of gestational diabetes primarily focuses on controlling blood sugar levels to reduce associated risks. This typically includes:
- Dietary Changes: A registered dietitian can help create a balanced meal plan that controls blood sugar levels.
- Regular Exercise: Staying active is important for managing gestational diabetes.
- Glucose Monitoring: Regularly testing blood sugar levels helps ensure they stay within the target range.
- Medication: In some cases, medication or insulin may be prescribed to help control blood sugar.
Prevention and Future Health
While not all cases of gestational diabetes can be prevented, there are steps pregnant women can take to reduce their risk. This includes maintaining a healthy weight, staying active, and consuming a balanced diet.
After giving birth, it's important for women who have had gestational diabetes to continue monitoring their health. This condition increases the risk of developing type 2 diabetes later in life. Regular check-ups and a healthy lifestyle can help mitigate this risk.
What are the risk factors for developing gestational diabetes during pregnancy?
Gestational diabetes can be effectively managed through diet and nutrition. This article provides comprehensive guidance on the dietary requirements and nutritional strategies to help expectant mothers control their blood sugar levels.
Understanding the Role of Diet in Managing Gestational Diabetes
Diet plays a pivotal role in the management of gestational diabetes. Controlling blood sugar levels is crucial to ensure the health and well-being of both the mother and the baby. Here are some essential dietary guidelines:
Balanced Carbohydrate Intake
Carbohydrates significantly affect blood sugar levels. Therefore, it's important to monitor carbohydrate intake. However, this doesn't mean eliminating carbs; rather, it involves choosing the right kinds of carbohydrates and managing portion sizes.
- Opt for complex carbohydrates like whole grains, fruits, and vegetables, as they have a lower impact on blood sugar.
- Spread carbohydrate intake throughout the day to maintain stable blood sugar levels.
- Avoid or limit high-sugar, refined carbohydrates like sugary snacks and beverages.
Protein for Sustained Energy
- Protein can help stabilize blood sugar and provide sustained energy. Including lean protein sources in your diet is essential.
- Lean meats, poultry, fish, and plant-based protein sources like tofu and legumes are excellent choices.
- Remember that a balanced diet includes a variety of proteins to ensure overall health.
Fiber-Rich Foods
- Fiber aids in blood sugar control and helps prevent blood sugar spikes. High-fiber foods are also beneficial for digestion.
- Include plenty of fiber-rich foods like whole grains, fruits, vegetables, and legumes.
- Fiber can help you feel full, reducing the temptation to overeat.
Healthy Fats
- Incorporating healthy fats into your diet is essential for overall health. These fats can also help stabilize blood sugar.
- Sources of healthy fats include avocados, nuts, seeds, and olive oil.
- Limit saturated and trans fats found in fried foods and processed snacks.
Meal Timing and Portion Control
- Eating at regular intervals and controlling portion sizes can help manage blood sugar levels effectively.
- Aim for three balanced meals and three small snacks throughout the day.
- Measuring portions and following a meal schedule can prevent overeating.
Blood Sugar Monitoring
- Regularly monitoring blood sugar levels is crucial for understanding how different foods affect your body. This information can guide dietary choices and help maintain stable blood sugar levels.
- Your healthcare provider will provide guidance on when and how to test your blood sugar.
- Record and share your results with your healthcare team to adjust your dietary plan as needed.
Hydration
- Staying hydrated is important for overall health, and it can also help control blood sugar levels.
- Water is the best choice for staying hydrated.
- Limit sugary beverages and excessive caffeine, which can affect blood sugar and hydration.
Seeking Professional Guidance
Managing gestational diabetes through diet and nutrition can be complex. It's advisable to work with a registered dietitian or nutritionist who specializes in gestational diabetes to create a personalized meal plan. They can provide guidance on specific foods, portion sizes, and meal timing based on your individual needs.
How does gestational diabetes affect both the mother and the baby?
Exercise and physical activity play a significant role in managing gestational diabetes. This article explores the importance of staying active during pregnancy and provides guidance on safe and effective exercise routines for expectant mothers with gestational diabetes.
Understanding the Benefits of Exercise During Pregnancy
Maintaining an active lifestyle during pregnancy offers numerous benefits for both the mother and the baby. For women with gestational diabetes, regular exercise can help control blood sugar levels, manage weight, and improve overall health. Here are some key advantages:
- Blood Sugar Control: Physical activity helps the body use insulin more effectively, leading to better blood sugar management.
- Weight Management: Exercise can assist in maintaining a healthy weight during pregnancy, reducing the risk of complications.
- Improved Mood: Physical activity releases endorphins, which can enhance mood and reduce stress.
- Increased Energy: Regular exercise can boost energy levels and combat pregnancy fatigue.
Consulting Your Healthcare Provider
Before starting any exercise program during pregnancy, it's essential to consult your healthcare provider. They can provide guidance tailored to your specific needs and circumstances. They will help determine the appropriate level of exercise and any precautions you should take.
Safe and Effective Exercises for Gestational Diabetes
- Walking: Brisk walking is a safe and accessible exercise for most pregnant women. It's a great way to get moving without putting too much stress on your joints.
- Swimming: Swimming and water aerobics are gentle on the joints and provide an excellent full-body workout.
- Prenatal Yoga: Prenatal yoga classes can help improve flexibility, strength, and relaxation. They often include modified poses suitable for pregnancy.
- Low-Impact Aerobics: Low-impact aerobic classes designed for pregnant women can offer an effective cardiovascular workout.
- Strength Training: Light strength training with proper form can help build muscle and improve metabolism. Focus on low weights and higher repetitions.
- Pilates: Prenatal Pilates can enhance core strength, flexibility, and posture. Make sure the instructor is qualified in prenatal fitness.
Exercise Precautions
While exercise is beneficial, it's essential to take specific precautions during pregnancy, especially if you have gestational diabetes:
- Stay hydrated before, during, and after exercise.
- Wear comfortable, breathable clothing and supportive footwear.
- Avoid overheating and exercise in a well-ventilated area.
- Listen to your body and don't overexert yourself. If you experience pain, dizziness, or shortness of breath, stop exercising immediately.
- Exercise Schedule
- The American College of Obstetricians and Gynecologists recommends at least 150 minutes of moderate-intensity aerobic activity spread throughout the week. This can be broken down into 30-minute sessions, five days a week.
Monitoring Blood Sugar
For women with gestational diabetes, monitoring blood sugar before and after exercise is crucial. You'll want to ensure that exercise isn't causing blood sugar levels to drop too low. A small, balanced snack before exercising may help maintain stable blood sugar.
Cooling Down and Stretching
After each exercise session, it's essential to cool down and perform stretching exercises. This can help prevent muscle soreness and improve flexibility. Gentle stretching can also promote relaxation.
Can gestational diabetes be managed through diet and exercise alone?
While many women with gestational diabetes can manage their condition through diet and exercise, some may require medication or insulin to control their blood sugar levels effectively. This article provides insights into medication and insulin management during pregnancy.
When Medication or Insulin Is Necessary
Gestational diabetes can vary in severity, and not all cases require medication or insulin. If dietary and lifestyle changes alone are insufficient to maintain target blood sugar levels, healthcare providers may recommend one or more of the following options:
- Oral Medications: Some women may be prescribed oral medications, typically metformin or glyburide, to help lower blood sugar.
- Insulin Injections: In cases where oral medications are ineffective or not recommended, insulin injections may be necessary.
- Combination Therapy: In some instances, a combination of oral medications and insulin may be used to achieve blood sugar control.
Monitoring Blood Sugar
Women taking medication or insulin for gestational diabetes must carefully monitor their blood sugar levels. This involves regular blood glucose testing at home. The results help ensure that the treatment plan is working effectively.
Dosing and Timing
The dosing and timing of medication or insulin are critical for managing gestational diabetes. Your healthcare provider will determine the appropriate dosage and schedule based on your blood sugar levels and specific needs. It's essential to follow the prescribed regimen precisely.
Potential Risks and Benefits
Using medication or insulin during pregnancy carries certain risks and benefits. It's essential to weigh these factors and discuss them with your healthcare provider.
Benefits:
- Blood Sugar Control: Medication or insulin can help achieve and maintain target blood sugar levels, reducing the risks associated with gestational diabetes.
- Healthier Pregnancy: Effective management of blood sugar levels can lead to a healthier pregnancy, with fewer complications for both the mother and the baby.
Risks:
- Hypoglycemia: Medication or insulin can lower blood sugar levels, potentially causing hypoglycemia (low blood sugar). This condition can be managed by consuming a small amount of fast-acting sugar, like fruit juice or glucose tablets.
- Weight Gain: Some individuals may experience weight gain when taking certain medications or insulin. It's essential to discuss these concerns with your healthcare provider.
Diet and Medication/Insulin
Women using medication or insulin must continue following a balanced diet that aligns with their treatment plan. Your healthcare provider or a registered dietitian can help you adjust your meal plan to accommodate medication or insulin.
Consulting Your Healthcare Provider
If you are prescribed medication or insulin for gestational diabetes, it's crucial to maintain open communication with your healthcare provider. Regular check-ups and discussions about your progress and any concerns are essential.
Birth Planning and Medication/Insulin
As your due date approaches, your healthcare provider will work with you to plan for labor and delivery. The use of medication or insulin may require adjustments during this time. Your healthcare team will ensure that you and your baby receive the necessary care.
What is the role of glucose monitoring in managing gestational diabetes?
Gestational diabetes doesn't end with childbirth; it can have implications for both the mother and the baby after delivery. This article explores the importance of postpartum monitoring and management of gestational diabetes.
Postpartum Blood Sugar Monitoring
After giving birth, it's crucial for women who had gestational diabetes to continue monitoring their blood sugar levels. While blood sugar levels often return to normal after childbirth, there is an increased risk of developing type 2 diabetes in the future.
Your healthcare provider will establish a schedule for blood sugar testing, which may involve oral glucose tolerance tests at specific intervals. This monitoring helps identify any potential changes in blood sugar levels and guides further management.
Breastfeeding and Gestational Diabetes
Breastfeeding is highly beneficial for both the mother and the baby, and it can also have a positive impact on blood sugar control. Breastfeeding can help improve insulin sensitivity and aid in the reduction of weight gained during pregnancy.
It's important for women with gestational diabetes to discuss their breastfeeding plans with their healthcare provider. Managing blood sugar levels during breastfeeding is crucial, and adjustments to meal planning or medication may be necessary.
Postpartum Weight Management
Gaining excessive weight during pregnancy is a risk factor for gestational diabetes. After giving birth, managing weight is essential to reduce the risk of developing type 2 diabetes.
Incorporating a balanced diet and regular exercise into your postpartum routine can help maintain a healthy weight. Consulting with a registered dietitian or a healthcare provider can assist in creating a personalized plan.
Family Health and Diabetes Prevention
A family approach to health is crucial in preventing diabetes in both the mother and the child. Encouraging a healthy lifestyle that includes nutritious meals and physical activity can be beneficial for the entire family.
Follow-Up Care
Regular follow-up care with your healthcare provider is essential. It provides an opportunity to assess your overall health, including blood sugar levels, and discuss any concerns or challenges you may be facing.
Understanding the Risk of Recurrence
While gestational diabetes typically resolves after giving birth, it increases the risk of developing type 2 diabetes in the future. Close monitoring and a proactive approach to health can help mitigate this risk.
Planning for Future Pregnancies
If you plan to have more children, it's important to discuss your history of gestational diabetes with your healthcare provider. They can provide guidance on managing and reducing the risk of recurrence in future pregnancies.
Are there any potential complications or long-term effects of gestational diabetes?
Managing gestational diabetes extends beyond the physical aspect; it also encompasses the psychological well-being of expectant mothers. This article explores the emotional aspects of dealing with gestational diabetes and offers coping strategies.
The Emotional Impact of Gestational Diabetes
A diagnosis of gestational diabetes can trigger a range of emotions, including worry, fear, and stress. The uncertainty about how the condition may affect both the mother and the baby can be overwhelming. It's essential to acknowledge and address these emotions.
Coping Strategies
Education and Understanding: The more you know about gestational diabetes, its management, and potential outcomes, the better equipped you'll be to cope with it. Attend educational sessions, speak with your healthcare provider, and seek information from reputable sources.
- Support System: Lean on your support network, including family, friends, and fellow expectant mothers who may have experienced gestational diabetes. Sharing your concerns and seeking emotional support can be immensely helpful.
- Stress Reduction: Stress management techniques such as deep breathing exercises, meditation, and mindfulness can help reduce anxiety and maintain emotional well-being.
- Focus on Positivity: Maintain a positive outlook by concentrating on the well-being of your baby and the positive changes you're making to manage gestational diabetes.
- Set Realistic Goals: Establish realistic goals for managing your condition, such as following your dietary plan, staying active, and monitoring your blood sugar levels.
- Consult a Mental Health Professional: If you find yourself struggling with persistent anxiety or depression related to gestational diabetes, consider consulting a mental health professional who can provide coping strategies and support.
Managing Fear and Anxiety
Fear and anxiety are common emotional responses to a gestational diabetes diagnosis. Here are some strategies to manage these emotions:
- Information Gathering: Understand that knowledge is empowering. Learning more about gestational diabetes and its management can help reduce fear.
- Consultation: Speak openly with your healthcare provider about your concerns and fears. They can provide guidance and reassurance.
- Support Groups: Joining a gestational diabetes support group can connect you with others experiencing similar emotions. Sharing your fears with those who understand can be comforting.
The Impact on Relationships
A diagnosis of gestational diabetes can also affect your relationships. Open communication with your partner is essential. They can be a valuable source of emotional support during this time. It's important to discuss how you both can work together to manage the condition.
Final Thoughts
In conclusion, gestational diabetes is a temporary condition that requires comprehensive care and attention during pregnancy. Understanding the causes, risks, and management of gestational diabetes is vital for expectant mothers. It involves a multifaceted approach, including diet and nutrition, exercise, potential medication or insulin management, and postpartum monitoring. Emotional well-being is equally important, and coping strategies can help manage the psychological impact of this condition.
By following the guidance of healthcare providers, maintaining a balanced lifestyle, and seeking support, women with gestational diabetes can successfully navigate this journey, ensuring a healthier pregnancy and birth. While gestational diabetes poses challenges, it also offers an opportunity for positive changes in lifestyle and a foundation for future health and well-being. With vigilance, support, and education, gestational diabetes can be managed effectively, resulting in a positive outcome for both the mother and the baby.
Related:
- Delicious and Nutritious: Gestational Diabetes Snacks Made Easy - Life Health
- Shocking Truth About COVID Pneumonia Survival Rate! You Won't Believe What the Numbers Reveal!
- Life Health: 12 Ways to Prevent Breast Cancer that Women Need to Know!
.png)

.png)


0 Comments